A New Direction in Healthcare Design
Healthcare design is shifting rapidly as providers search for more efficient ways to meet the growing demand for outpatient healthcare services.


Washington Health Urgent Care – Fremont, CA
Across the industry, design firms are seeing a strong move toward adaptive reuse converting commercial offices, gyms, and older healthcare facilities into modern outpatient environments. Ware Malcomb is seeing this trend firsthand through projects such as the San Diego Rescue Mission transformation and multiple Neighborhood Healthcare renovations, as well as new work with a confidential investment company to reimagine recently acquired office properties for medical use. This shift is driven by multiple factors: the high cost of ground‑up construction, the availability of underused building stock after COVID, and the growing need for community‑based care settings that do not require the complexity of a full hospital.

Romeo Orthopaedics – Burr Ridge, IL
Healthcare clients are increasingly broadening their perspective on where care can be delivered, exploring opportunities to repurpose non‑healthcare buildings for medical and behavioral health use. This shift presents exciting possibilities but also introduces challenges, including navigating entitlements, addressing parking requirements, and adapting base building layouts not originally designed for hands‑on evaluation, ongoing therapy, or team‑based support. These factors are prompting clients to rethink how interior spaces can be reconfigured to support essential clinical functions. Several facility layout strategies have emerged as effective solutions for medical office buildings, including behavioral health settings. Each approach balances privacy, safety, supervision, workflow, and patient experience in ways that reflect evolving healthcare delivery models, reimbursement pressures, and community needs.
Linear Layout
This is the layout that most people recognize from traditional medical offices. A public waiting area sits at the entrance, exam or therapy rooms are located beyond it, and staff or administrative spaces are positioned behind those rooms. Patients and staff share the same hallways, creating a familiar and approachable environment.
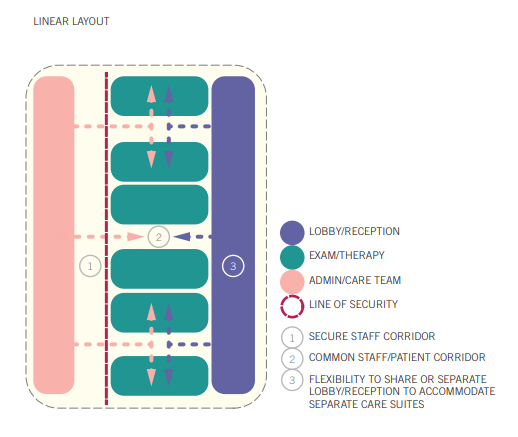
The experience is straightforward: patients check in, are escorted to their room, settle in, and wait briefly for their provider. Shared circulation encourages casual interactions and helps maintain a strong sense of connection between patients and care teams.
For behavioral health, this layout is especially flexible. Therapy rooms can feel more like offices or living rooms rather than clinical exam spaces, which helps put patients at ease. The standard exam layout works best when there is no need for dual access or increased supervision, and when comfort, dignity, and simplicity are the primary goals.
On-stage/ Off-stage Layout
This model introduces a clear separation between public and private circulation. Patients access exam or therapy rooms from the “on-stage” side typically the waiting area and patient-facing corridor while staff use a secured “off-stage” corridor. These rooms often have two doors, allowing providers to enter and exit without crossing patient pathways.
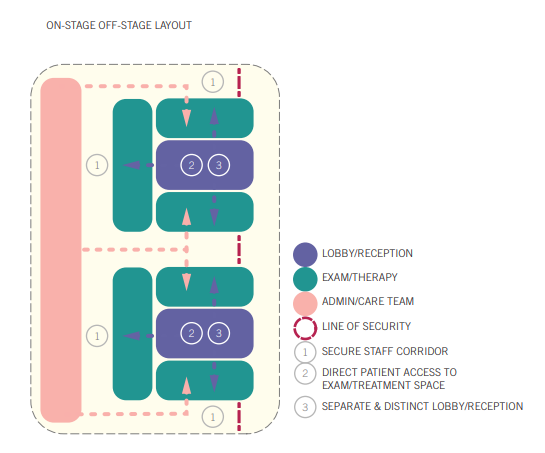
This setup enhances privacy and creates more controlled movement throughout the clinic. It reduces unplanned interactions in hallways and focuses all patient–provider engagement inside the exam room itself. For behavioral health, this layout can be especially beneficial. If a patient is experiencing increased distress or agitation the second exit provides an added layer of safety for care teams. Providers can leave discretely if needed, and the room becomes the primary interaction zone, supporting calm, intentional conversations.
The on-stage/off-stage model also helps create a dignified patient experience by clearly defining where care happens and reducing exposure to staff workflows. It’s well‑suited for outpatient behavioral health programs, medical clinics with higher‑acuity needs, or facilities where privacy and safety are high priorities.
Pod-Based Layout
This approach centralizes the care team in a shared work hub, with exam or consultation rooms positioned along the perimeter. Staff have constant visibility of all room entrances, which supports supervision, communication, and coordination.
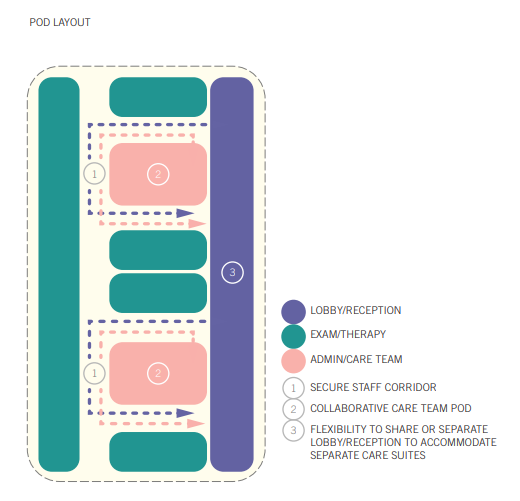
This layout is extremely effective for integrated care. Many clinics especially those serving underserved populations operate as “one‑stop‑shop” models where patients may see a therapist, a medical provider, a nutritionist, and even receive legal or social services support in one visit. Having the entire care team grouped in a central zone allows them to collaborate in real time, discuss patient needs, and coordinate next steps quickly.
Because staff can see the entire corridor and all room entries, this layout also offers a higher level of oversight. It is especially helpful in behavioral health environments where patients may need guidance moving from one service to another, or where staff need visual awareness to maintain safety. This layout supports warm hand-offs, team‑based care planning, and a seamless patient experience that reduces barriers particularly for communities that often have difficulty accessing or navigating healthcare systems.
The Path Forward
As healthcare continues to shift toward more accessible, community‑based care, adaptive reuse is becoming a key strategy for expanding outpatient services. Offices, gyms, and older hospital buildings present valuable opportunities to deliver high‑quality care by transforming existing structures into modern healthcare environments.
The three layout types discussed – Linear Layout, On-stage/ Off-stage Layout, Pod-Based Layout – offer distinct advantages depending on patient populations, staffing models, safety requirements, and the level of integrated care. As providers continue to adapt to new reimbursement structures, community needs, and post‑COVID space availability, these design strategies will help shape the next generation of medical and behavioral health facilities. By understanding how each approach functions, organizations can make design decisions that support dignity, safety, collaboration, and the evolving realities of modern healthcare.


